 A high ventilatory ratio was also associated with increased mortality (OR, 1.55 95% CI, 1.33-1.80 p < 0.001 I2 = 48%). After adjusting for other confounding variables, every 0.05 increase in pulmonary-dead space fraction was associated with an increased odds of death (OR, 1.23 95% CI, 1.13-1.34 p < 0.001 I2 = 57%). 
A high pulmonary dead-space fraction was associated with increased mortality (odds ratio, 3.52 95% CI, 2.22-5.58 p < 0.001 I2 = 84%). We included 28 studies in our review, 21 of which were included in our meta-analysis. The quality and strength of evidence were assessed using the Quality in Prognostic Studies and Grading of Recommendations, Assessment, Development, and Evaluation, respectively. We calculated pooled effect estimates using a random effects model for both adjusted and unadjusted results. Two reviewers independently identified eligible studies and extracted data. Studies including adults with ARDS reporting a dead-space ventilation index and mortality. MEDLINE, CENTRAL, and Google Scholar from inception to November 2022. 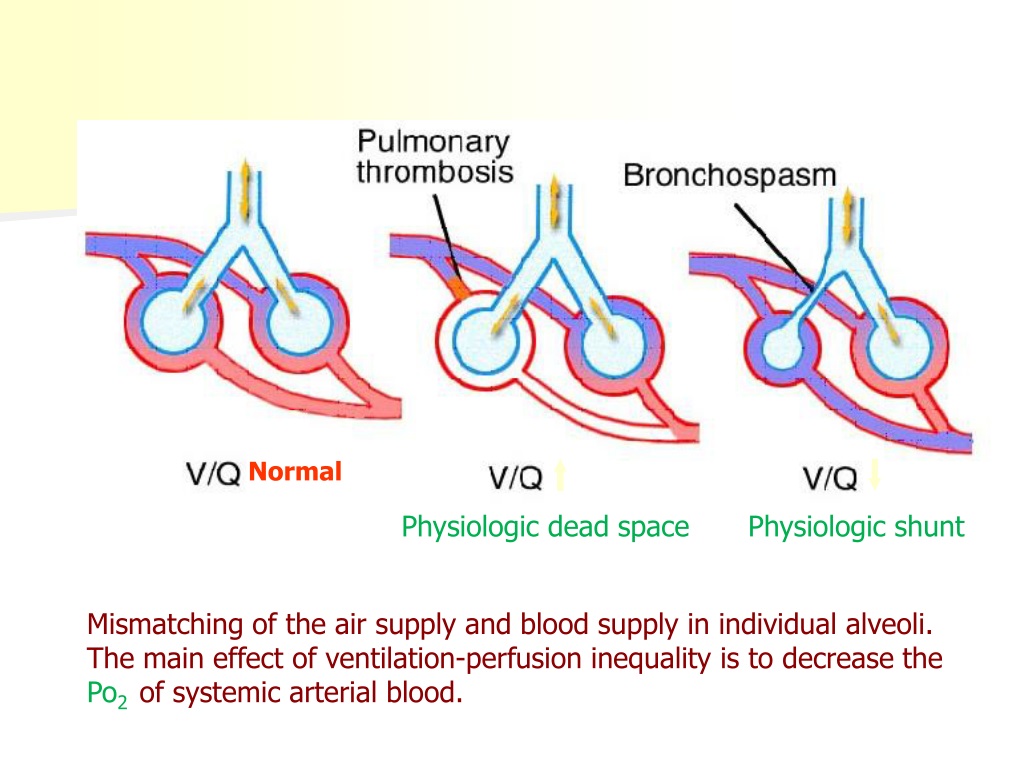
In this systematic review and meta-analysis, we evaluated the ability of dead-space ventilation measures to predict mortality in patients with ARDS. However, whether the degree of dead-space ventilation is associated with outcomes is uncertain. Acute respiratory distress syndrome (ARDS) is associated with high ventilation-perfusion heterogeneity and dead-space ventilation. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
